Ask the Flight Surgeon / By Dr. (LTC) Joseph Puskar: A recent case study of an air traffic controller who developed type II (neurologic) decompression sickness (DCS) after a series of four consecutive training SCUBA dives illustrates the dangers of DCS for military and civilian divers and aviators.
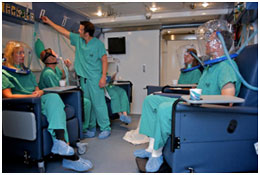
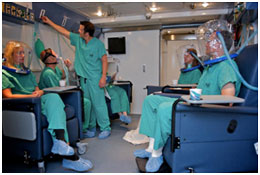 Soldiers inside the hyperbaric chamber wearing oxygen masks.Aircraft designed and built specifically for military usage require lengthy schedules for design, manufacturing, and testing. A relatively small production quantity results in a high unit cost. When Army operational requirements can be satisfied by modifying a readily available COTS aircraft, the warfighter is provided with a modern system quickly and economically.
Soldiers inside the hyperbaric chamber wearing oxygen masks.Aircraft designed and built specifically for military usage require lengthy schedules for design, manufacturing, and testing. A relatively small production quantity results in a high unit cost. When Army operational requirements can be satisfied by modifying a readily available COTS aircraft, the warfighter is provided with a modern system quickly and economically.
The affected individual is a highly experienced SCUBA instructor diver and final approach radar operator who developed severe type II DCS ninety minutes after surfacing from his fourth dive over thirty feet in less than three hours. Symptoms included shoulder joint and muscle pain, vertigo, ataxia, right eye ptosis, and vision changes including double vision and worsening tunnel vision that progressed to complete right eye blindness.
He immediately went to the nearest medical facility with a hyperbaric chamber, but was told there that he was most likely having a stroke, and was not put in the chamber despite his concerns that it was DCS, and calling the Divers’ Alert Network (DAN) emergency number. He was admitted to the hospital’s medical floor under the care of neurology for stroke workup, and was finally transferred to a large university medical center hyperbaric facility five days post injury after a thorough workup by neurology and ophthalmology. It was found that a micro-embolism had severely damaged the left 8th cranial nerve causing imbalance with a tendency to fall to the right, left spinning vertigo upon looking up, and severe tinnitus, or ringing of the ear.
A retired Navy dive medical officer at the chamber facility immediately pressed him in the chamber on a USN treatment table 6 protocol, and the right eye blindness completely resolved. The other symptoms also gradually improved although not completely after ten treatments, and he was discharged with vestibular training and antivert (meclizine) for the vertigo. Initial attempts to man the radar scope caused severe vertigo, nausea, and vomiting obviating his return to work. After a series of chronic phase hyperbaric oxygen treatments at lower pressures and over a few months however, his symptoms gradually resolved, and he was happily able to return to ATC duties with a waiver.
What is DCS
Decompression sickness (DCS) is caused by the formation of inert gas bubbles in tissues and blood after saturation where the mechanical stresses caused by bubbles or their secondary cellular effects cause organ dysfunction. There are several mechanisms by which bubbles exert their harmful effects. These include direct mechanical disruption of tissue, occlusion of blood flow, platelet deposition and activation of the coagulation cascade, endothelium dysfunction, capillary leakage, endothelial cell death, complement activation, and leukocyte activation and inflammation.
Treatment
Hyperbaric oxygen therapy is the most definitive treatment for this disorder. It has several benefits including immediate reduction in bubble volume, increasing the diffusion gradient for the nitrogen into the blood and interstitial fluid, and ultimately out the lungs, oxygenation of ischemic tissue, and reduction of central nervous system (CNS) edema. In later phases of treatment hyperbaric oxygen has other beneficial effects including reduction in neutrophil adhesion to the capillary endothelium reducing the secondary inflammatory effects that persist even after the nitrogen bubbles have resolved. Hyperbaric oxygen therapy has been shown to benefit DCS symptoms up to two weeks after the initial injury, and chronic phase injury may benefit from even longer courses of therapy, so treatment is done until there is no further improvement in symptoms.
Safety First
Repetitive dives such as this diver’s five dive training day, even though well within the limits of conservative dive tables, always increase the risk for decompression sickness, and the same can be said of repetitive high altitude flights. A relatively recent spate of increased high altitude pressurized aircraft DCS in military pilots that included some severe and permanently disabling cases were ultimately found to be due to an overly ambitious number of sorties in the flight schedule that did not allow enough time for complete physiologic recuperation between flights. Keep in mind that no dive tables or high altitude flight profiles are completely safe, and the original U.S. Navy dive tables were written with an expectation of an approximately six percent DCS rate in fit young divers.
If you suspect you may be having type II, or any other form of DCS, contact your nearest flight surgeon or diving medicine officer, and get the hyperbaric oxygen treatment that you need if it’s indicated. Oxygen administered at sixty feet of seawater pressure is the quickest way to off-gas harmful nitrogen bubbles that may have formed, and every hour of delay in getting to a chamber diminishes the odds of successfully treating the condition and returning to flight duty without any residual deficits.
Question for the Flight Surgeon?
If you have a question you would like addressed, email it to This email address is being protected from spambots. You need JavaScript enabled to view it.; we’ll try to address it in the future. See your unit flight surgeon for your personal health issues. The views and opinions offered are those of the author and researchers and should not be construed as an official Department of the Army position unless otherwise stated.
Dr. (LTC) Joseph Puskar is a flight surgeon at the U.S. Army Aeromedical Center, Fort Rucker, AL.