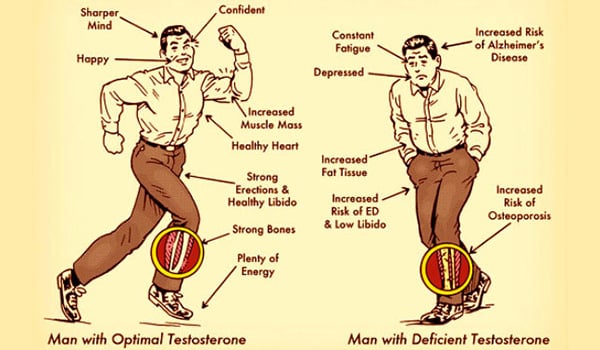
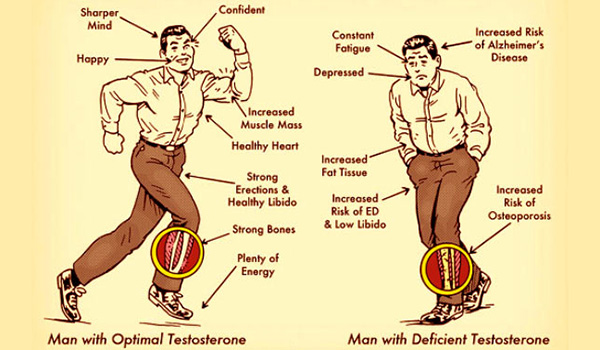
Ask the Flight Surgeon / By MAJ Jason MacDonnell, M.D.: Q: Lately I have heard a lot about the symptoms of low testosterone in men. Who should be tested and if there is a problem, how is it treated?
>
FS: With the increase in direct to consumer advertising and men’s specialty clinics, the access to treatments like testosterone therapy are on the rise. In fact, over the past decade the use of testosterone has more than tripled in the U.S. Before pursuing a long-term treatment like hormone replacement, patients should understand the risks and benefits to make an informed decision. Testosterone is part of a group of hormones called androgens and is one of the most important sex hormones in men. The brain controls the production and release of testosterone from the testicles into the bloodstream. The function of this hormone is complex, affecting several areas of the body to include the cardiovascular, neurologic and musculoskeletal systems.
Who should be tested?
It is easy to find websites that list the symptoms of low testosterone. Many patients come to the clinic with low sex drive, fatigue, muscle weakness and a decrease in mood or cognition wondering if it could be related to their testosterone level. While these are symptoms related to low hormone levels, they could also be related to other conditions that are equally likely to be present. This is why a thorough history and physical is always the first place to start. Other medical conditions like diabetes, obstructive sleep apnea and depression affect the production of testosterone, so reviewing all your past medical issues with the provider is important. If the clinical picture is suggestive of a testosterone deficiency, then ordering lab work is appropriate.
How is the test performed?
Blood levels of testosterone fluctuate and can vary from hour to hour throughout the day. The level peaks in the morning and drops to a low point by the afternoon. This is why the provider will ask for a morning blood sample, usually between 7-9 A.M. Some providers might ask that you fast, similar to a cholesterol test. This is due to research that shows sugar ingestion can decrease testosterone levels. If your levels are found to be below the threshold for normal, national guidelines suggest that a confirmatory blood test be completed before the decision to treat is made. There is a growing market of home testing kits but these should be avoided. The results can be hard to interpret, their accuracy cannot be guaranteed and there might be other conditions present that are impacting your health.
If my levels are low, how is it treated?
Treatment is recommended for symptomatic men by replacing testosterone with a goal of improvement of symptoms. Over the years there have been several forms of delivery for testosterone replacement to include, injections, patches, topical gels, skin implants and oral tabs. While these are all considered to be acceptable routes, one might be more appropriate than another for a particular patient. Work with your provider to determine the right choice of treatment for you. Many patients ask about one of the several over-the-counter testosterone boosters that have flooded the market. None of these have been tested for efficacy and could be harmful in the long run. It is important to remember that testosterone treatment does have potential risks; there is concern for increased risk of stroke, heart attack and blood clots. Treatment could also be contraindicated in patients with obstructive sleep apnea, urinary symptoms or an increase in the number of red blood cells.
Can I get a waiver if I am put on testosterone?
Most often men with low testosterone are diagnosed with a condition called Hypogonadism. While this can be for many different reasons, a majority of men have age-related failure of the testis. While there is not a specific aeromedical policy letter on this condition, starting a new medication is reason for temporary grounding. The flight concern includes the symptoms that are present (such as poor concentration, weakness or fatigue) and any potential side effects of starting hormone replacement. Once there is a reversal of symptoms with no signs of side effects, a waiver can be requested and is routinely granted. Ongoing monitoring of this condition would then be included as part of the annual flight physical for continuation of the waiver.
Issues discussed in mass media can spark a conversation with your provider but should not be the guiding force of your healthcare. If you are having any of the issues mentioned above, bring them up to your Doc and get them treated. Timely identification and workup of issues facilitates the waiver process and minimizes downtime.
Questions?
If you have a question you would like addressed, email it to This email address is being protected from spambots. You need JavaScript enabled to view it.; we’ll try to address it in the future. See your unit flight surgeon for your personal health issues. The views and opinions offered are those of the author and researchers and should not be construed as an official Department of the Army position unless otherwise stated.
MAJ (Dr.) Jason MacDonnell is a flight surgeon at the U.S. Army School of Aviation Medicine, Fort Rucker, AL.