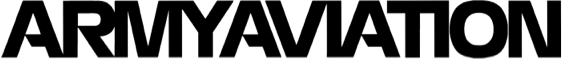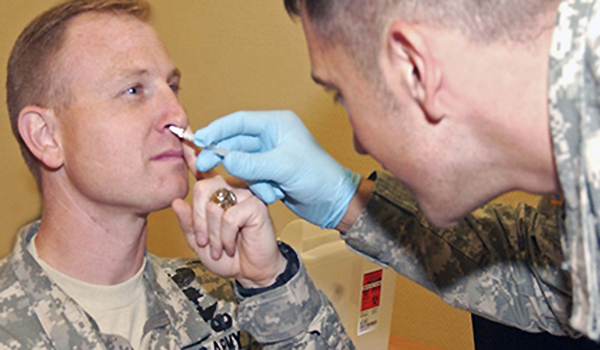
Ask the Flight Surgeon / By CPT Gurdeep Buttar, M.D.: Q: I’m a 26 year old pilot, who just moved to Ft. Rucker, Alabama for specialized training. I’ve always had seasonal allergies, but this year has been the worst. I have a runny nose, nasal congestion, and a nagging cough. I think I need something stronger than over-the-counter medications, but I am concerned that prescription medications may make me drowsy in the cockpit. What options do I have to treat my allergies, but still be safe flying?
FS: Seasonal allergies are a very common health concern whose symptoms present when your immune system overreacts to an outdoor substance that your body is sensitized to (an “allergen”), such as pollen. Symptoms of seasonal allergies can be numerous, including itchy, watery eyes, fullness in the ears, sneezing, as well the concerns you described. In fact, your runny nose, also known as seasonal allergic rhinitis (SAR), is estimated to affect 15-30% of Americans in any given year. SAR can lead to sleepless nights, decreased concentration and unproductive or missed time at work and in the cockpit. Though numerous over the counter medications are available to help reduce the symptoms of SAR, not all of these medications are safe for use in flight or interact well with other medications you may be taking or other health concerns you may have.
The presence of SAR shows a strong interconnection with a form of eczema called atopic dermatitis as well as overgrowth of the lining of your nasal cavity known as nasal polyps. SAR is also strongly associated with asthma. In fact, the majority of patients with asthma present with symptoms of SAR or perennial allergic rhinitis. SAR is a global health issue with considerable economic and societal burdens to the sufferer. It is estimated that people with SAR see their health care provider 1.8 times more often than people that do not have the condition and use twice as much medication.
When individuals are exposed to an allergen, SAR symptoms can present within minutes. Diagnosis of SAR is often made in the primary care clinic. However, diagnosis is not always straightforward as SAR symptoms can be very much like symptoms of other common problems. So, your medical provider will be careful during the examination to help rule out other causes such as non-allergic rhinitis and viral infections such as the common cold. When talking to your provider, also make sure to describe your work, home, and hobby environments. The use of a new product at work, the adoption of a pet, or the start of a home improvement project may be affecting your symptoms and could change how your health concerns are managed.
The type of treatment prescribed for SAR is based on the nature of the symptoms. Seasonal, episodic, or mild symptoms may be relieved with oral or nasal anti-histamines combined with a short acting decongestant. Mild symptoms may also be helped with simple, daily nasal saline rinses that flush out the sinuses. Moderate symptoms may require additional medications like intranasal steroids, anti-histamine eye drops, or medications that improve breathing. Severe allergies may require allergen immunotherapy that consists of a series of allergy shots meant to buildup tolerance to allergens and reduce the extent of the symptoms. Be sure to coordinate all care with your aeromedical provider as therapies like immunotherapy injections require temporary grounding periods to monitor for unwanted reactions.
If a trial with standard therapies is ineffective, a more specific diagnosis may be determined by an Allergy/Immunology specialist to better direct therapy. In this instance, allergen-specific skin testing and/or blood tests may be indicated. Skin testing uses small amounts of suspected allergens that are gently placed under the skin’s surface. Skin tests generally produce rapid results while blood tests that look for allergen-specific antibodies may take several days to process.
Untreated SAR can be hazardous in-flight. SAR can produce swelling and obstruction of the soft tissues of the nasal passages and throat leading to an increase risk of sinus and ear blocks at altitude. Furthermore, over-the-counter allergy treatments, even antihistamines labeled as “non-sedating,” can cause various levels of drowsiness and some nasal sprays can worsen symptoms if used improperly. Of the over-the-counter anti-histamines, only fexofenadine and loratadine may be waived if used on a long-term basis (30+ days per year). Therapy requiring oral steroids, immunotherapy, or sinus surgery may require a waiver to continue flying. Standard therapy for mild to moderate symptoms does not prohibit pilots from flying, but you should always consult with your aeromedical provider. If you are experiencing SAR symptoms, do not hesitate to get evaluated as there are many options to lessen or even eliminate your symptoms and keep you flying.
Fly safe!
Question?
If you have a question you would like addressed, email it to This email address is being protected from spambots. You need JavaScript enabled to view it..”>This email address is being protected from spambots. You need JavaScript enabled to view it.. We will try to address it in the future. See your unit flight surgeon for your personal health issues. The views and opinions offered are those of the author and researchers and should not be construed as an official Department of the Army position unless otherwise stated.
CPT (Dr.) Gurdeep Buttar is a flight surgeon at the School of Army Aviation Medicine, Fort Rucker, AL.